Over 120 million Americans are missing at least one tooth, and that number grows by 2 million annually. Yet here’s what’s striking: while tooth loss has historically been viewed as an inevitable part of aging, modern dental implant technology has fundamentally changed that narrative. Today’s implants achieve success rates exceeding 95% and can last decades with proper care – making them not just a treatment option, but often the gold standard for tooth replacement.
The shift toward implants reflects broader changes in how we understand oral health. Research from the Journal of Dental Research shows that tooth loss triggers immediate bone deterioration, affecting facial structure and adjacent teeth within months. Traditional solutions like dentures and bridges, while helpful, don’t address this underlying biological process. Dental implants, however, actually preserve and stimulate jawbone health by mimicking natural tooth roots.
For the millions facing tooth loss decisions, understanding these differences isn’t academic—it’s deeply personal. The choice between replacement options affects not just appearance, but daily functions like eating, speaking, and long-term oral health. Whether you’re dealing with a single missing tooth or considering full-mouth reconstruction, the science behind implants reveals why they’ve become the preferred solution for patients who qualify.
Here’s what current research and clinical experience tell us about how implants work, who benefits most, and what factors should guide your decision-making process.
What Are Dental Implants and Why Do They Matter?
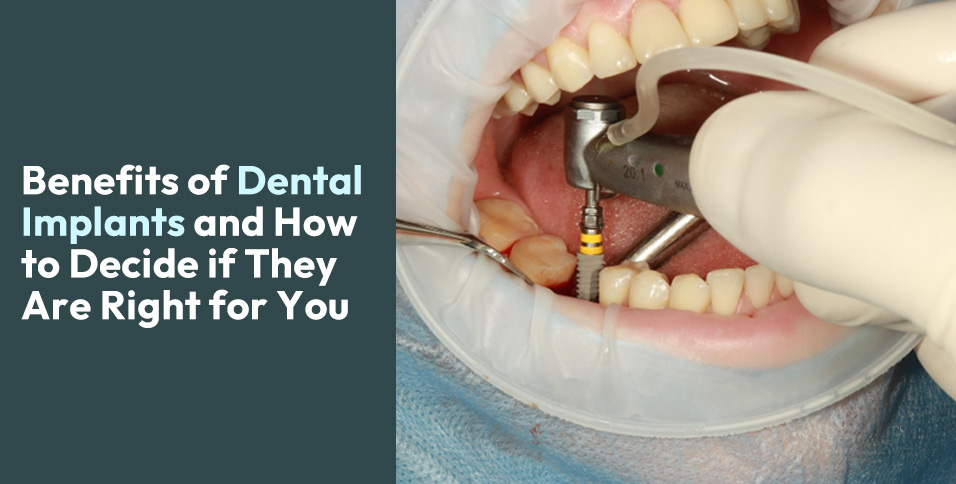
Dental implants represent a fundamental shift from traditional tooth replacement approaches. Unlike dentures that sit on top of gums or bridges that rely on adjacent teeth for support, implants integrate directly with your jawbone to create an artificial tooth root. This titanium post, typically 3-5mm in diameter, serves as the foundation for a crown that looks and functions like your natural tooth.
The biological advantages become clear when you understand what happens after tooth loss. Within the first year, the jawbone in that area loses up to 25% of its width due to lack of stimulation. This process, called resorption, continues throughout life and explains why denture wearers often develop that characteristic “sunken” facial appearance over time. The bone simply disappears without the mechanical stress that tooth roots normally provide.
Implants interrupt this destructive cycle by delivering the same mechanical forces to your jawbone that natural teeth do. When you chew, the implant transfers those forces directly to the bone, maintaining its density and structure. This preservation effect extends beyond the implant site—it helps maintain the position and health of neighboring teeth that might otherwise shift or become compromised.
From a functional standpoint, implants restore nearly 100% of natural chewing efficiency, compared to 25-50% for conventional dentures. Patients report being able to eat previously avoided foods like corn on the cob, apples, and nuts without concern about slippage or discomfort. The psychological impact proves equally significant: surveys consistently show that implant patients experience greater confidence in social and professional situations compared to those with removable appliances. For individuals researching treatment options, consulting specialists who provide dental implants in Atlanta can help determine whether implants are the most appropriate solution for restoring both function and long-term oral health.
The integration process that makes these benefits possible relies on a biological phenomenon that wasn’t well understood until the 1950s, when Swedish orthopedic surgeon Per-Ingvar Brånemark accidentally discovered osseointegration during titanium research.
How Do Dental Implants Integrate With the Jawbone?
Osseointegration—the direct structural and functional connection between living bone and the implant surface—represents one of modern medicine’s most remarkable healing processes. Unlike other medical implants that remain separate from surrounding tissue, dental implants actually become part of your jawbone at the cellular level.
The process begins immediately after implant placement. Your body recognizes the titanium surface as biocompatible and begins depositing new bone cells directly onto it. Within days, specialized cells called osteoblasts start laying down a matrix of proteins that will eventually mineralize into mature bone. This isn’t scar tissue formation or encapsulation—it’s actual bone growth that creates a mechanical bond stronger than many natural materials.
The timeline follows a predictable pattern that varies based on bone quality and location. In the dense bone of the lower jaw, primary stability occurs within 6-8 weeks, while complete integration takes 3-4 months. Upper jaw integration typically requires 4-6 months due to less dense bone structure. During this period, patients wear temporary restorations that protect the healing implant from excessive force while maintaining function and aesthetics.
Modern implant surfaces enhance this natural process through micro-texturing and chemical treatments. Research published in Clinical Oral Implants Research demonstrates that these surface modifications can increase bone-to-implant contact by up to 85%, compared to 60-70% for smooth surfaces. Some manufacturers add calcium phosphate coatings that further accelerate integration by providing a scaffold for bone formation.
The strength of this biological bond becomes apparent in long-term studies. After complete integration, implants can withstand chewing forces of 200-250 pounds per square inch—comparable to natural teeth. This durability explains why properly placed implants routinely function for 25-30 years or longer, often outlasting the crowns they support.
However, successful integration depends on maintaining precise surgical protocols and patient factors that influence bone healing. Understanding these variables helps explain why not everyone qualifies for immediate implant placement, and why the process sometimes requires preliminary procedures.
What Types of Dental Implants Are Available?
The dental implant landscape has evolved far beyond the standard “one-size-fits-all” approach of early systems. Today’s options encompass different designs, materials, and placement protocols tailored to specific clinical situations and patient needs.
Endosteal implants represent the most common type—titanium screws placed directly into the jawbone. These come in various diameters (3.5-6mm) and lengths (8-16mm) to accommodate different anatomical situations. Standard diameter implants (4-4.5mm) work well for most applications, while narrow implants (3.5mm) serve areas with limited space, and wide implants (5-6mm) provide enhanced stability in posterior regions with significant chewing forces.
Subperiosteal implants offer an alternative for patients with insufficient bone height who cannot undergo bone grafting procedures. These custom-fabricated metal frameworks sit on top of the jawbone but under the gum tissue, providing support for multiple teeth. While less common today due to advances in bone grafting techniques, they remain valuable for specific cases where conventional implants aren’t feasible.
Material science has introduced zirconia implants as an alternative to titanium, particularly appealing to patients with metal sensitivities or those preferring metal-free solutions. Zirconia’s white color eliminates the gray show-through that can occur with titanium implants in thin gum tissue areas. However, zirconia implants require careful case selection due to their brittleness compared to titanium’s flexibility.
Immediate load protocols allow crown placement on the same day as implant surgery, dramatically reducing treatment time from months to hours. This approach works best in cases with excellent bone quality and adequate primary stability. Studies show success rates of 95-98% for immediate loading in suitable candidates, though careful patient selection remains critical.
Delayed loading remains the gold standard for complex cases, compromised bone quality, or situations requiring bone grafting. This traditional approach allows complete osseointegration before adding the restoration, maximizing long-term success rates even in challenging situations.
The choice between these options depends on factors like bone quality, gum tissue thickness, aesthetic requirements, and patient preferences regarding treatment timeline versus predictability. Understanding these trade-offs helps explain why thorough evaluation precedes any implant treatment plan.
How Do Dental Implants Compare to Dentures and Bridges?
The comparison between implants and traditional tooth replacement options reveals fundamental differences in approach, function, and long-term consequences that extend far beyond initial cost considerations.
Functional performance shows the starkest contrasts. Complete dentures typically restore only 25-30% of natural chewing efficiency, limiting food choices and affecting nutrition. Partial dentures perform better at 50-60%, but still require dietary modifications. Traditional bridges restore 80-90% of function, though this depends entirely on the health of supporting teeth. Implants consistently deliver 95-100% of natural function, allowing unrestricted diet and normal eating patterns.
Bone preservation represents perhaps the most significant long-term difference. Dentures accelerate bone loss through uneven pressure distribution and lack of root stimulation. Studies tracking denture wearers over 15 years show an average of 4-6mm of vertical bone loss, requiring frequent adjustments and eventual denture replacement. Bridges preserve bone only under the pontic (artificial tooth), while the extraction sites continue deteriorating. Implants actively maintain bone through mechanical stimulation, actually improving bone density in many cases.
Impact on adjacent teeth varies dramatically between approaches. Dentures typically require clasps that place stress on remaining teeth, potentially loosening them over time. Traditional bridges demand removing healthy enamel from adjacent teeth to create crowns, permanently altering these teeth and making them more susceptible to decay and fracture. Implants stand independently, preserving neighboring teeth completely.
Maintenance requirements follow different patterns for each option. Dentures need nightly removal for cleaning, special adhesives for retention, and periodic professional adjustments. They typically require replacement every 5-7 years due to bone changes and wear. Bridges require special flossing techniques and are vulnerable to decay at crown margins, with average lifespans of 10-15 years. Implants require only routine brushing and flossing like natural teeth, with proper maintenance enabling decades of service.
Comfort and stability differences become apparent during daily use. Well-fitting dentures can slip during speaking or eating, causing embarrassment and limiting confidence. Bridges feel more natural but can trap food and create cleaning challenges. Implants feel identical to natural teeth, with no movement or special considerations during use.
These functional differences explain why patient satisfaction surveys consistently rank implants highest among tooth replacement options, despite higher initial investment. The question for most patients becomes whether they qualify for implant treatment and can manage the process requirements.
Who Is a Good Candidate for Dental Implants?
Implant candidacy depends on multiple biological, medical, and behavioral factors that influence both immediate surgical success and long-term stability. Understanding these criteria helps explain why comprehensive evaluation precedes any implant treatment plan.
Bone quality and quantity serve as the primary determining factors. Successful osseointegration requires adequate bone height, width, and density to support the implant during healing and function. Cone beam CT scans reveal three-dimensional bone architecture, identifying areas where natural bone suffices versus locations requiring grafting procedures. Patients with severe bone loss from prolonged tooth absence may need bone augmentation before implant placement, extending treatment time but enabling successful outcomes.
Gum health provides the foundation for long-term implant stability. Active periodontal disease must be controlled before implant surgery, as the same bacteria that destroy natural tooth support can cause implant failure through peri-implantitis. Patients with a history of gum disease require ongoing periodontal maintenance to maintain implant health, but successful treatment doesn’t disqualify them from implant therapy.
Systemic health considerations influence healing capacity and infection risk. Well-controlled diabetes doesn’t preclude implant treatment, but uncontrolled blood sugar levels impair bone healing and increase complication rates. Smoking significantly reduces success rates—studies show 85-90% success in non-smokers versus 70-75% in smokers—due to reduced blood flow and impaired healing. Many clinicians require smoking cessation before proceeding with implant surgery.
Age factors work in both directions. Younger patients need completed jaw growth—typically age 18-21—before implant placement, as continuing growth can alter implant position. Older patients face no upper age limit if they’re healthy enough for routine dental procedures. In fact, many octogenarians successfully receive implants with outcomes comparable to younger patients.
Medication considerations can affect candidacy. Bisphosphonate medications for osteoporosis carry a small risk of osteonecrosis, requiring careful evaluation and possible drug holidays before surgery. Blood thinners necessitate coordination with physicians but don’t automatically disqualify patients. Immunosuppressive medications require individual assessment based on specific drugs and dosages.
Behavioral factors influence long-term success significantly. Patients who maintain excellent oral hygiene and attend regular dental visits achieve the highest success rates. Those with habits like teeth grinding may need protective nightguards to prevent implant complications. Unrealistic aesthetic expectations or unwillingness to follow post-operative instructions can compromise outcomes.
The evaluation process typically reveals that most adults qualify for implant treatment, though the timeline and complexity vary based on individual circumstances. Understanding potential risks and maintenance requirements becomes equally important for making informed decisions.
What Are the Risks and Maintenance Requirements of Dental Implants?
Like any surgical procedure, dental implant placement carries inherent risks that, while uncommon, require understanding for informed decision-making. Current research indicates overall complication rates of 5-10%, with most issues being minor and manageable.
Immediate surgical risks include infection, bleeding, and nerve damage. Infection occurs in fewer than 2% of cases when proper sterile technique and antibiotic protocols are followed. Excessive bleeding is rare in healthy patients but can occur with certain medications or bleeding disorders. Nerve damage, particularly to the inferior alveolar nerve in the lower jaw, affects less than 1% of cases when proper surgical planning and imaging are used. Temporary numbness may occur but permanent damage is extremely uncommon.
Implant failure manifests in two primary forms. Early failure, occurring within the first few months, typically results from poor bone quality, inadequate healing, or infection. This affects 2-5% of implants and usually requires removal and replacement after healing. Late failure, developing years after successful integration, often stems from peri-implantitis—an inflammatory condition similar to gum disease around natural teeth.
Peri-implantitis represents the most significant long-term risk, affecting 10-15% of implant patients over 10 years. This condition occurs when bacteria accumulate around the implant, causing gum inflammation and eventual bone loss. Risk factors include poor oral hygiene, smoking, diabetes, and previous gum disease. Early detection through regular professional monitoring enables successful treatment, but advanced cases may require implant removal.
Mechanical complications involve prosthetic components rather than the implant itself. Screw loosening affects 5-10% of implants, usually manifesting as crown mobility or unusual sensations. This typically represents a minor adjustment rather than a serious problem. Crown fractures occur in fewer than 5% of cases, usually from excessive forces or material fatigue over time.
Maintenance requirements for implants mirror those for natural teeth but require specific considerations. Daily brushing and flossing remain essential, though special tools may be needed around implant crowns. Interdental brushes, water flossers, and implant-specific floss help maintain cleanliness around restoration margins. Professional cleanings every 3-6 months allow monitoring for early signs of complications and removal of deposits that home care cannot eliminate.
Long-term monitoring enables early intervention when problems develop. Annual X-rays track bone levels around implants, while clinical examinations assess gum health and prosthetic stability. Patients with risk factors like diabetes or previous gum disease may require more frequent monitoring to maintain optimal outcomes.
The key insight from long-term studies is that most complications are preventable through proper patient selection, surgical technique, and ongoing maintenance. Patients who maintain excellent oral hygiene and attend regular appointments achieve success rates exceeding 95% over decades of function.
What Does Research Show About Dental Implant Success and Future Trends?
Clinical research spanning over 50 years provides compelling evidence for dental implant effectiveness, with recent studies revealing success rates and longevity that continue improving as techniques and technology advance.
Long-term success data from multiple large-scale studies demonstrates remarkable durability. The Swedish national registry, tracking over 200,000 implants for up to 30 years, reports 95% survival rates at 10 years and 90% at 20 years. American studies show similar patterns, with success rates varying by location—mandibular implants achieving 98% success versus 95% for maxillary implants, reflecting differences in bone density.
Age-related outcomes reveal that success rates remain consistent across adult age groups. A 2023 study in the International Journal of Oral and Maxillofacial Implants found no significant difference in success between patients aged 65-75 versus those aged 45-55, provided systemic health was comparable. This challenges earlier assumptions about age limitations and supports implant treatment for healthy older adults.
Technology advances are reshaping implant treatment protocols. Digital planning software now enables virtual implant placement before surgery, improving precision and reducing complications. Guided surgery systems translate computer planning into precise surgical execution, with studies showing improved accuracy and reduced surgical time. Three-dimensional printing enables custom surgical guides and immediate temporary restorations, streamlining the treatment process.
Surface technology innovations continue improving osseointegration speed and quality. Hydrophilic surfaces, created through specialized treatments, accelerate early bone formation by up to 50% compared to traditional surfaces. Bioactive coatings containing bone morphogenetic proteins show promise for enhancing integration in compromised bone situations. These advances may eventually reduce healing times while maintaining or improving success rates.
Immediate loading protocols have expanded significantly as research identifies ideal conditions for same-day function. Studies now support immediate loading for single teeth, multiple units, and even full-arch reconstructions in carefully selected cases. Success rates for immediate loading approach those of conventional protocols when proper criteria are met, offering patients faster restoration of function and aesthetics.
Future developments suggest continued evolution in materials and techniques. Zirconia implants are being refined to address brittleness concerns while maintaining biocompatibility advantages. Stem cell research explores possibilities for regenerating bone and soft tissues around implants. Nanotechnology applications may enable surfaces that actively promote healing while resisting bacterial colonization.
Artificial intelligence is beginning to influence treatment planning and outcome prediction. Machine learning algorithms analyze thousands of cases to identify factors associated with success or failure, potentially enabling more precise patient selection and treatment modifications. Predictive models may soon help clinicians optimize treatment protocols for individual patients based on their specific risk profiles.
The trajectory of implant research suggests that current excellent outcomes will continue improving as technology and understanding advance. For patients considering implants today, this research foundation provides confidence in choosing a treatment approach with decades of scientific validation and continuous refinement.
The evidence consistently points to dental implants as more than a tooth replacement option—they represent a comprehensive approach to preserving oral health and function. As techniques continue evolving and success rates climb even higher, the question for most patients shifts from whether implants work to whether their individual situation makes them the optimal choice. The combination of proven long-term success, ongoing technological advances, and expanding treatment options suggests that implant dentistry will continue setting the standard for tooth replacement in the decades ahead.