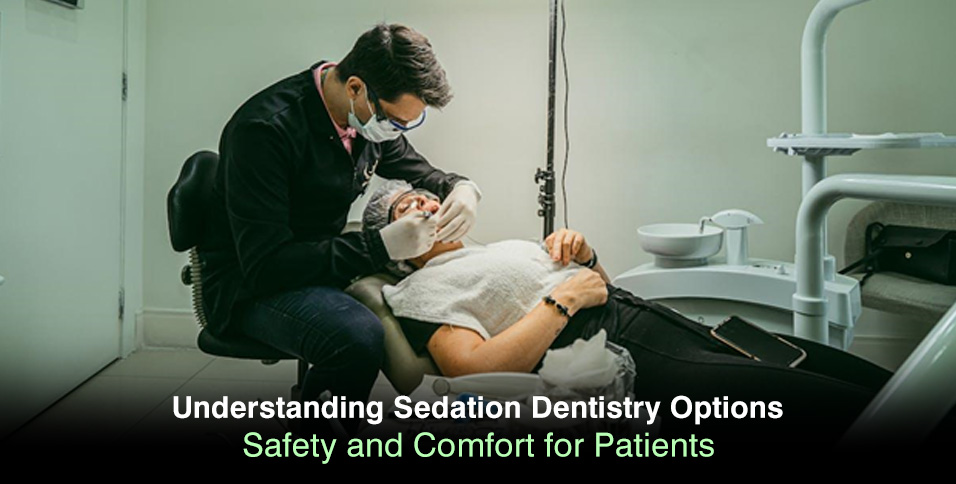
Nearly 36% of Americans experience dental anxiety, with 12% suffering from extreme dental phobia that prevents them from seeking necessary care. This anxiety crisis has real health consequences—people delay treatments until emergencies develop, leading to more complex procedures and higher costs. What’s particularly striking is that 78% of those who avoid dental visits cite fear of pain or discomfort as their primary concern, yet modern sedation techniques can virtually eliminate these issues.
The landscape of dental sedation has transformed dramatically in recent years. Advanced monitoring systems, refined medication protocols, and better patient screening have made sedation dentistry safer and more accessible than ever before. Where once only oral surgeons offered these services, general dentists now routinely provide various gentle sedation options, making anxiety-free dental care available to millions more patients.
For the one in three adults who struggle with dental anxiety, understanding these sedation options isn’t just about comfort—it’s about accessing the preventive and restorative care that protects their overall health. The choice between enduring anxiety or receiving treatment no longer exists. Here’s how modern sedation dentistry works and what options can transform your dental experience.
What Is Sedation Dentistry and How Does It Work?
Sedation dentistry uses medications to help patients relax during dental procedures, creating a state where anxiety dissolves and discomfort becomes manageable. Unlike local anesthesia, which only blocks pain sensation in specific areas, sedation affects your central nervous system to reduce anxiety, fear, and awareness of the procedure.
The medications work by enhancing the activity of gamma-aminobutyric acid (GABA), a neurotransmitter that naturally calms brain activity. When GABA receptors are activated, they slow down nerve transmission, creating feelings of relaxation and reducing the brain’s response to stress and fear. This neurological shift allows patients to remain conscious and responsive while feeling deeply relaxed and detached from any discomfort.
Sedation levels exist on a spectrum from minimal to deep. Minimal sedation keeps you awake but relaxed—you might feel like you’ve had a glass of wine. Moderate sedation, often called “conscious sedation,” creates a deeper relaxation where you may slur words or not remember much of the procedure. Deep sedation brings you to the edge of consciousness, where you can still be awakened but likely won’t remember the treatment.
The key advantage is that sedation doesn’t replace pain management—it works alongside local anesthesia. While the local anesthetic prevents physical pain, sedation addresses the psychological component of dental anxiety. This dual approach means you experience neither the physical discomfort nor the emotional distress that typically accompanies dental procedures.
Understanding these mechanisms helps explain why sedation works so effectively for dental anxiety. Your brain’s natural alarm systems quiet down, allowing you to receive necessary care without the fight-or-flight response that normally makes dental visits so challenging.
Types of Sedation Dentistry Used in Dental Care
Modern dental practices offer four primary sedation methods, each delivering different levels of relaxation through distinct administration routes. The choice depends on your anxiety level, the procedure’s complexity, and your medical history.
Nitrous oxide, commonly known as laughing gas, provides the mildest form of sedation. You breathe a mixture of nitrous oxide and oxygen through a small mask placed over your nose. The effects begin within minutes—you’ll feel relaxed and slightly euphoric, but remain fully conscious and able to respond to instructions. The gas leaves your system quickly once the mask is removed, usually within five minutes.
Oral sedation involves taking prescribed medication before your appointment, typically benzodiazepines like triazolam or diazepam. Depending on the dosage, oral sedation can range from minimal to moderate levels. You’ll feel drowsy and deeply relaxed, though you’ll remain awake. Many patients report feeling like they slept through the procedure, even though they were responsive throughout.
Intravenous (IV) sedation delivers medications directly into your bloodstream through a small needle in your arm or hand. This method allows precise control over sedation levels, as your dentist can adjust the medication dosage in real-time. IV sedation typically produces moderate to deep sedation levels, with most patients having little to no memory of the procedure.
General anesthesia renders you completely unconscious and is typically reserved for complex oral surgeries or patients with severe medical conditions. Under general anesthesia, you cannot be easily awakened until the effects wear off, and you’ll require specialized monitoring equipment and trained anesthesia providers.
Each method offers distinct advantages in terms of onset time, duration, and depth of sedation, making it crucial to match the right option to your specific needs and comfort level.
How Nitrous Oxide and Oral Sedation Differ
Nitrous oxide and oral sedation represent the two most common entry points into sedation dentistry, yet they create fundamentally different experiences for patients. Understanding these differences helps you choose the option that best matches your anxiety level and treatment needs.
Nitrous oxide works almost immediately—within two to three minutes of breathing the gas, you’ll notice a floating sensation and decreased anxiety. The effects remain consistent throughout your procedure because you’re continuously breathing the medication. Most patients describe feeling euphoric, slightly light-headed, and completely relaxed while maintaining full awareness of their surroundings. You can communicate normally with your dental team and follow instructions without difficulty.
The major advantage of nitrous oxide is its reversibility. Once the mask comes off and you breathe pure oxygen for a few minutes, the effects disappear completely. You can drive yourself home and return to normal activities immediately. This makes it ideal for routine cleanings, fillings, or other shorter procedures where you want anxiety relief without significant impairment.
Oral sedation creates a deeper, longer-lasting effect that begins 30-60 minutes after taking the medication. The experience feels more like drowsiness than euphoria—many patients compare it to being very sleepy or having taken a strong sleep aid. While you remain conscious and can respond to questions, your reactions may be slower, and your memory of the procedure will likely be hazy or completely absent.
The trade-off with oral sedation is the extended recovery period. The medication continues affecting you for several hours after your appointment, requiring someone to drive you home and stay with you until the effects fully wear off. However, this deeper level of sedation makes it excellent for longer procedures, multiple treatments in one visit, or patients with moderate to severe dental anxiety.
Your dentist can combine oral sedation with nitrous oxide for even deeper relaxation when needed, creating a customized approach that matches your specific anxiety level and treatment requirements.
Intravenous Sedation and General Anesthesia Explained
For patients requiring deeper sedation or undergoing complex procedures, intravenous sedation and general anesthesia represent the most profound levels of relaxation and unconsciousness available in dental settings.
IV sedation provides what many consider the “gold standard” for conscious sedation in dentistry. Once the IV line is established in your arm, medications like midazolam or propofol flow directly into your bloodstream, creating almost immediate effects. Unlike other sedation methods, your dentist can adjust the medication level throughout the procedure, deepening or lightening your sedation as needed.
Most patients under IV sedation enter a twilight state—deeply relaxed but still breathing independently and responding to verbal commands. Time perception disappears almost entirely; what feels like minutes to you may actually be hours of dental work. The amnesia effect is so pronounced that 90% of patients report remembering nothing about their procedure, even though they were cooperative and responsive throughout.
The monitoring requirements for IV sedation are extensive. Your blood pressure, heart rate, oxygen levels, and breathing patterns are continuously tracked by specialized equipment. A trained sedation team member stays with you throughout the procedure, separate from the dentist performing your treatment. This level of monitoring ensures your safety while maintaining the deep relaxation that makes complex procedures comfortable.
General anesthesia takes sedation to its deepest level, rendering you completely unconscious. In dental settings, this typically occurs in hospital operating rooms or specialized surgical centers equipped with advanced life support systems. You’ll be intubated to maintain your airway, and an anesthesiologist will manage your breathing and vital signs throughout the procedure.
General anesthesia is reserved for the most complex cases: full-mouth reconstructions, multiple wisdom tooth extractions, jaw surgeries, or patients with severe medical conditions that make conscious sedation inappropriate. The recovery process is more involved, requiring several hours of monitoring as you wake up and regain full consciousness.
The distinction between conscious sedation (IV) and unconscious sedation (general anesthesia) is crucial. With IV sedation, you maintain protective reflexes and can breathe on your own. Under general anesthesia, these functions require medical support, which explains why the setting and personnel requirements differ so significantly between these two approaches.
Safety Considerations and Patient Monitoring During Sedation
The safety of sedation dentistry depends on comprehensive patient evaluation, appropriate medication selection, and continuous monitoring throughout the procedure. Modern sedation protocols have established safety records that rival those of routine medical procedures when properly administered.
Pre-procedure evaluation begins with a detailed medical history focusing on conditions that might complicate sedation. Heart disease, breathing disorders, liver problems, and certain medications can affect how your body processes sedation drugs. Your dentist will review all medications you’re taking, including over-the-counter supplements, as some can interact dangerously with sedation medications. Allergies to specific drug classes must be identified and avoided.
Age and weight significantly influence medication dosing. Elderly patients typically require lower doses and experience longer recovery times due to slower metabolism. Pediatric sedation requires specialized training and different medication protocols entirely. Your dentist calculates precise dosages based on your body weight, medical conditions, and the planned procedure length.
During the procedure, monitoring intensity varies by sedation level. Nitrous oxide requires basic vital sign checks and visual monitoring. Oral sedation demands more frequent blood pressure and oxygen level measurements. IV sedation requires continuous electronic monitoring of heart rhythm, blood pressure, oxygen saturation, and breathing patterns. A pulse oximeter clips to your finger, a blood pressure cuff cycles automatically, and breathing sensors track your respiratory rate.
Emergency preparedness is essential for any sedation practice. Dental offices providing sedation maintain emergency medications like flumazenil (which reverses benzodiazepine effects) and equipment for airway management. Staff receive training in basic life support and sedation emergency protocols. Most importantly, they know when to stop a procedure and seek emergency medical assistance.
Common side effects include drowsiness, dizziness, and nausea, particularly with oral and IV sedation. These typically resolve within hours as the medication clears your system. More serious complications like allergic reactions or respiratory depression are rare but require immediate medical intervention. This is why proper patient screening and continuous monitoring are non-negotiable aspects of safe sedation practice.
Recovery protocols ensure you don’t leave the office until you meet specific safety criteria: stable vital signs, alertness appropriate for your sedation level, and the presence of a responsible adult to drive you home and monitor your continued recovery.
Benefits of Sedation Dentistry and Its Role in Pain and Anxiety Management
Beyond simply reducing anxiety, sedation dentistry transforms the entire dental experience by addressing both psychological and physiological barriers to care. The benefits extend far beyond the dental chair, impacting long-term oral health outcomes and overall quality of life.
Psychological benefits are perhaps the most profound. Patients with dental phobia often develop a cycle where anxiety about dental visits leads to avoidance, which allows problems to worsen, creating more complex and potentially painful procedures that reinforce their fears. Sedation breaks this cycle by creating positive dental experiences. Research shows that 89% of patients who receive sedation dentistry report reduced anxiety about future dental visits, even for procedures without sedation.
The memory effects of sedation play a crucial role in anxiety reduction. Because many patients remember little or nothing about their sedated procedures, they don’t develop traumatic memories that could worsen future dental anxiety. This “amnesia benefit” allows anxious patients to receive necessary care without accumulating negative associations with dental treatment.
Pain management improves significantly with sedation, even though sedation medications don’t directly block pain. When you’re relaxed and anxiety-free, your pain threshold increases naturally. Muscle tension decreases, breathing becomes deeper and more regular, and your body’s stress response diminishes. This physiological relaxation makes local anesthesia more effective and reduces the amount of pain medication needed.
Sedation also enables longer appointments, allowing dentists to complete multiple procedures in single visits. Instead of requiring four separate appointments for four dental crowns—each causing anxiety—sedation allows all four crowns to be completed in one relaxed session. This efficiency reduces overall treatment time, minimizes disruption to your schedule, and decreases cumulative anxiety exposure.
Special populations benefit enormously from sedation options. Children with dental anxiety can receive necessary treatments without developing lasting fears about dental care. Elderly patients with mobility issues or cognitive impairment can remain comfortable during longer procedures. Patients with disabilities that make cooperation difficult can receive comprehensive care that might otherwise be impossible.
The ripple effects extend beyond dental health. When dental anxiety no longer prevents regular care, patients maintain better oral health, which connects to improved cardiovascular health, better diabetes control, and reduced risk of systemic infections. The confidence that comes from knowing you can receive comfortable dental care often leads to more proactive healthcare engagement overall.
Research on Effectiveness and Future Trends in Sedation Dentistry
Current research demonstrates that sedation dentistry not only improves patient comfort but also enhances treatment outcomes and practice efficiency. A 2024 study published in the Journal of Dental Research found that patients receiving sedation dentistry showed 67% better appointment compliance and 45% fewer emergency visits compared to those relying on local anesthesia alone.
Safety data continues to support sedation dentistry’s excellent track record. Analysis of over 50,000 sedation cases from the American Dental Association’s sedation registry shows serious adverse events occurring in fewer than 0.02% of procedures—comparable to routine medical procedures. The key factors in maintaining this safety record include proper training, appropriate patient selection, and adherence to monitoring protocols.
Effectiveness studies reveal compelling benefits beyond anxiety reduction. Patients undergoing sedated procedures report significantly lower perceived pain levels even when receiving identical local anesthesia protocols. This suggests that anxiety reduction creates measurable improvements in pain perception, validating the dual approach of sedation plus local anesthesia for optimal comfort.
Emerging trends in sedation dentistry focus on precision and personalization. Pharmacogenetic testing—analyzing how your genes affect drug metabolism—is beginning to inform sedation protocols. Some patients metabolize benzodiazepines rapidly and need higher doses, while others process these medications slowly and require careful monitoring to prevent over-sedation. Genetic testing can predict these variations, allowing for more precise dosing.
Technology integration is revolutionizing sedation monitoring. Next-generation pulse oximeters can detect subtle changes in oxygen levels minutes before traditional devices. Continuous capnography, which measures exhaled carbon dioxide, is becoming standard for moderate sedation cases. These advances provide earlier warning signs if patients develop breathing difficulties.
Training standardization continues evolving with new simulation technologies. Dental schools now use high-fidelity mannequins that can simulate sedation emergencies, allowing students to practice emergency responses without patient risk. Continuing education requirements for practicing dentists are becoming more stringent, with many states mandating hands-on simulation training for sedation permit renewal.
The global trend toward sedation dentistry adoption is accelerating. European dental practices report 340% growth in sedation services over the past five years, while similar expansion occurs across Asia and South America. This worldwide adoption is driving innovation in sedation protocols and safety systems, creating a positive feedback loop that continues improving patient care.
Future developments include ultra-short-acting sedation medications that provide deep relaxation but clear from your system in minutes rather than hours. Research into targeted anxiety medications that specifically address dental-related fears without general sedation effects shows promise. Virtual reality integration with light sedation is being studied as a way to enhance relaxation while reducing medication requirements.
The trajectory is clear: sedation dentistry is becoming more precise, safer, and more widely available. For the millions of people who currently avoid dental care due to anxiety, these advances represent the difference between neglecting their oral health and receiving the care they need in comfort and confidence.