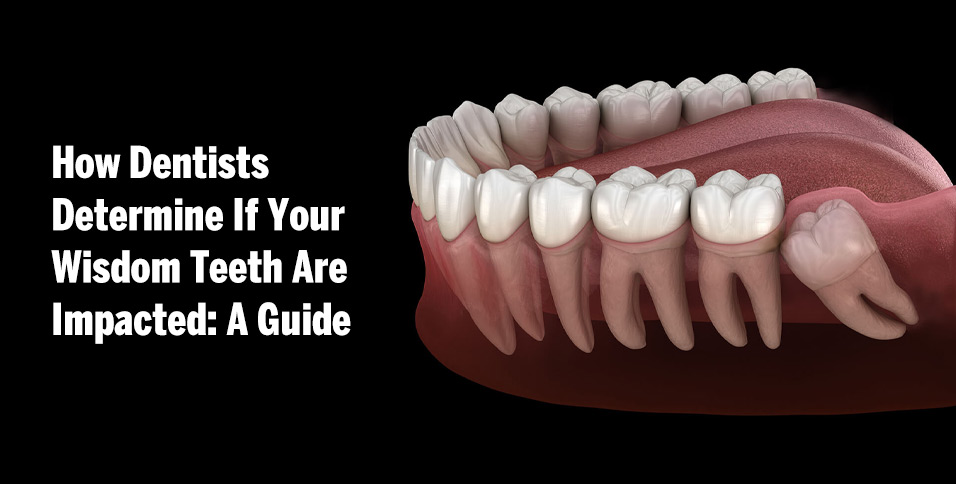
Wisdom teeth are the last set of molars to develop, usually emerging between the ages of seventeen and twenty-five. By the time they begin to erupt, however, the jaw has often already reached its full size. In many individuals, there simply isn’t enough space left for these teeth to grow properly. Therefore, a wisdom tooth may tilt sideways, remain partially buried in the gum, or stay trapped within the jawbone entirely. This situation is referred to as impaction.
Research highlights that impacted wisdom teeth are remarkably common, affecting more than a third of people worldwide. Notably, the prevalence appears even higher among Asian populations, where nearly half of individuals may have at least one impacted third molar.
Unfortunately, understanding whether a wisdom tooth is impacted requires more than simply looking inside the mouth. In fact, dentists rely on a careful combination of clinical examination, imaging, and experience to determine what is happening beneath the surface. This makes wisdom teeth removal a procedure that demands both precision and professional judgment.
If you’re wondering whether discomfort in your mouth points to an impacted wisdom tooth, read this guide before your dental consultation.
Step 1: Conducting an Initial Examination
Assessing the health of your wisdom teeth usually begins with a straightforward clinical examination. During the check-up, the dentist will examine the back of your mouth and evaluate the condition of the gums surrounding the third molars. At this stage, the goal is to see whether a tooth is visible and identify subtle warning signs that suggest the tooth may be erupting abnormally.
For example, swollen or inflamed gum tissue behind your second molar often signals that a wisdom tooth is attempting to break through but doesn’t have enough space to do so. Food debris trapped beneath a small flap of gum can also point toward partial eruption, which frequently leads to recurrent infection known as pericoronitis.
The dentist may also gently probe the area to assess how easily the region can be cleaned. When a wisdom tooth sits at an awkward angle, plaque tends to accumulate around it, increasing the risk of decay not only in the wisdom tooth but also in the neighbouring molar.
Step 2: Evaluating Other Subtle Symptoms
You may think that severe pain is the first sign of trouble, but dentists often detect impacted wisdom teeth long before symptoms become dramatic. As mentioned, swollen gum tissue may already indicate wisdom tooth problems. Another warning sign is persistent bad breath or an unpleasant taste in your mouth, which may indicate infection beneath the gum flap.
Jaw stiffness, difficulty opening the mouth fully, or pressure around the neighbouring molars may also suggest that a wisdom tooth is pushing against surrounding structures. These symptoms might seem minor at first, but they provide valuable clues during a dental evaluation.
Moreover, dentists pay close attention to these subtle patterns because early detection often allows treatment to occur before complications develop.
Step 3: Taking Dental X-Rays
While the physical examination provides useful clues, X-rays remain the most important tool for confirming whether a wisdom tooth is impacted. A panoramic dental X-ray allows the dentist to view your entire jaw in a single image, including teeth that have not yet erupted.
This imaging reveals several critical details. First, it shows the angle of the wisdom tooth in relation to the neighbouring molar. A tooth leaning forward into the second molar is one of the most common forms of impaction. In other cases, the tooth may grow horizontally or remain completely trapped within the bone.
Second, X-rays allow the dentist to assess how deeply the tooth sits within the jaw. A tooth positioned close to the surface of the gum is usually easier to remove than one embedded deep within the bone.
Third, the proximity of the tooth’s roots to the inferior alveolar nerve is another crucial detail that dentists study carefully before recommending surgery. This nerve runs through the lower jaw and provides sensation to your lower lip and chin. Because of its location, dentists must evaluate the relationship between the nerve and the wisdom tooth roots to minimise the risk of complications. Dental imaging helps guide this decision and ensures that you’re offered the safest treatment plan.
Step 4: Recognising the Type of Impaction
Once imaging is reviewed, dentists classify the impaction based on the position of the tooth. Understanding these positions helps determine whether removal is necessary and how complex the surgery may be.
For example, mesioangular impaction, where a tooth that tilts forward toward the second molar, is among the most frequently seen patterns. This type sometimes erupts partially, so surgeons will sometimes monitor the tooth to determine the best timing for surgery.
Another possibility is horizontal impaction, where the wisdom tooth lies completely sideways beneath the gum. In such a case, there’s no chance for the tooth to erupt normally and you will need immediate surgery.
Don’t Delay Your Consultation
If you suspect that your wisdom teeth may be causing your discomfort, it’s best to schedule a professional evaluation rather than waiting for the problem to worsen. With modern imaging and careful assessment, dentists in Singapore can usually determine quickly whether a wisdom tooth is impacted and whether treatment is necessary. In most cases, the consultation itself provides reassurance and a clear plan forward, helping you make the most responsive decisions about your oral health.