According to the American Dental Association’s 2024 clinical data, dental implants have a success rate exceeding 95% when placed by qualified practitioners — yet many patients approach the procedure with anxiety rooted in uncertainty about what actually happens during surgery. As digital imaging and minimally invasive techniques transform modern implantology, the patient experience has evolved significantly from the lengthy, uncomfortable procedures of even a decade ago.
For the estimated 178 million Americans missing at least one tooth, understanding the surgical process can mean the difference between informed confidence and unnecessary stress. The procedure itself typically unfolds over several months, but the actual surgical placement — the part that generates the most questions — usually takes between 60 to 90 minutes per implant. What happens during those crucial hours sets the foundation for years of restored function, and knowing what to expect can help patients navigate both the physical and emotional aspects of this life-changing treatment.
What Happens During the Dental Implant Procedure
The surgical appointment begins with local anesthesia administration, though many practices now offer sedation options for patients who prefer to remain more relaxed throughout the process. Your surgeon will inject a numbing agent around the implant site, often using a topical anesthetic first to minimize any discomfort from the injection itself. Within minutes, the area becomes completely numb, though you’ll remain awake and aware of pressure sensations.
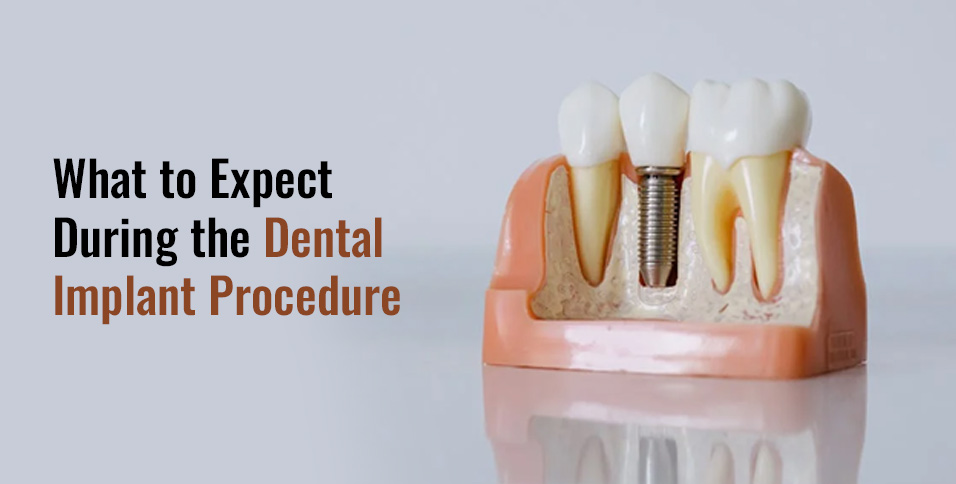
Once adequate numbness is confirmed, the surgeon creates a small incision in the gum tissue to access the underlying jawbone. Using specialized drills that operate at precise speeds and temperatures, they gradually create a pilot hole in the bone, then carefully widen it to match the implant’s diameter. The drilling sequence follows a specific protocol — starting with the smallest diameter and progressively increasing — to prevent overheating the bone tissue, which could compromise healing.
The titanium implant itself resembles a small screw, typically measuring between 3.5 to 6 millimeters in diameter and 8 to 16 millimeters in length, depending on your anatomy and the tooth being replaced. The surgeon places the implant using controlled force, ensuring it sits flush with or slightly below the bone surface. This precise positioning is critical for both immediate stability and long-term success.
After implant placement, the surgeon positions a healing cap or cover screw on top of the implant, then sutures the gum tissue closed. In some cases where immediate loading is planned, a temporary crown can be attached the same day, though this approach requires specific bone quality conditions. Most patients report feeling only pressure and vibration during the procedure, with actual pain being minimal thanks to modern anesthetic techniques.
How Should Patients Prepare for Dental Implant Surgery?
Successful implant surgery begins weeks before you enter the treatment room, with thorough preparation addressing both your systemic health and the surgical site itself. Your dental team will review your medical history in detail, paying particular attention to conditions that might affect healing — diabetes, autoimmune disorders, and medications like blood thinners or bisphosphonates all require careful consideration and possible modification of the treatment plan.
Pre-surgical instructions typically include avoiding smoking for at least two weeks before surgery, as nicotine dramatically reduces blood flow to the surgical site and increases failure risk. If you take blood-thinning medications, your physician may adjust the dosage temporarily, though this decision requires coordination between your dentist and medical doctor. The day before surgery, you’ll receive specific guidelines about eating and drinking, particularly if sedation is planned.
The morning of surgery, focus on maintaining normal routines while following any pre-operative instructions. Wear comfortable clothing and arrange for transportation if you’ve chosen sedation options beyond local anesthesia. Having all-on-X dental implants Philadelphia procedures often requires longer appointment times and more extensive preparation, particularly when multiple implants are being placed simultaneously to support a full arch restoration.
Who Is a Good Candidate for Dental Implants?
Ideal implant candidates combine adequate bone volume with good systemic health and realistic expectations about the treatment timeline. Your jawbone needs sufficient height, width, and density to support the implant — measurements determined through 3D cone beam CT scans that reveal bone architecture in detail. Adults of any age can receive implants, though the jaw must be fully developed, which typically occurs by the late teens.
Certain medical conditions don’t automatically disqualify you but require careful management. Well-controlled diabetes, for example, doesn’t prevent implant success, but blood sugar levels should remain stable throughout the healing period. Heavy smoking significantly increases failure risk, with success rates dropping from over 95% to around 85% in smokers. Radiation therapy to the head and neck region also complicates healing, though delayed placement protocols can still achieve success in many cases.
Gum disease must be treated and controlled before implant placement, as active infection creates an environment hostile to healing. Your periodontist will ensure your remaining teeth and gums are healthy, establishing the foundation for long-term implant success. Adequate bone quality — measured on a scale from D1 (very dense) to D4 (very soft) — influences both the surgical approach and healing timeline, with denser bone providing more immediate stability but potentially requiring longer integration periods.
What Are Common Risks and Complications After Surgery?
While implant surgery carries a high success rate, understanding potential complications helps you recognize warning signs and seek appropriate care when needed. Infection at the surgical site represents the most common immediate concern, typically manifesting as increased swelling, persistent throbbing pain, or unusual discharge after the first few days. Most infections respond well to antibiotic therapy when caught early, but delayed treatment can compromise the implant.
Implant failure occurs in roughly 2-5% of cases, with most failures happening either within the first few months due to poor initial integration, or years later due to peri-implantitis — an inflammatory condition similar to gum disease that affects the tissues around the implant. Early failure signs include mobility of the implant, persistent pain, or failure of the gum tissue to heal properly. Late failures often develop gradually, with symptoms including bleeding around the implant, bad taste, or loosening of the restoration.
Nerve damage, while rare, represents a serious potential complication, particularly with lower jaw implants placed near the inferior alveolar nerve. Temporary numbness affecting the lip, chin, or tongue occurs in fewer than 2% of cases, with permanent damage being exceptionally rare when proper planning and surgical technique are employed. Sinus complications can arise with upper jaw implants if the implant extends into the sinus cavity, though this typically resolves with appropriate management.
Some patients experience prolonged swelling or bruising beyond the normal healing timeline, particularly if they have underlying circulation issues or take certain medications. While these complications can be concerning, most resolve with conservative management and don’t affect the long-term implant success. The key lies in maintaining regular follow-up appointments and communicating any unusual symptoms promptly to your surgical team.
How Does Recovery Unfold After Dental Implant Placement?
The initial recovery period focuses on managing discomfort while protecting the surgical site from disruption. Most patients experience peak swelling and discomfort during the second and third days after surgery, with gradual improvement following. Ice packs applied for 15-20 minutes at a time during the first 24 hours help minimize swelling, while prescription or over-the-counter pain medications manage discomfort effectively for most people.
Dietary modifications play a crucial role in early healing, with soft foods recommended for the first week to avoid putting pressure on the implant site. Cold foods like ice cream or smoothies can provide comfort, while hot beverages and spicy foods should be avoided initially. Gentle rinsing with warm salt water beginning 24 hours after surgery helps keep the area clean without disturbing the healing tissues.
Activity restrictions typically include avoiding strenuous exercise for the first week, as increased blood pressure and heart rate can promote bleeding and swelling. Sleeping with your head elevated for the first few nights helps minimize overnight swelling. Most patients return to work within a day or two, though jobs requiring heavy physical activity may require a longer recovery period.
What Is the Typical Healing Timeline After Surgery?
The healing process unfolds in distinct phases, beginning with soft tissue healing over the first 2-3 weeks, followed by the crucial osseointegration period lasting 3-6 months. During the initial weeks, the gum tissue closes around the healing cap, and any sutures dissolve or are removed. You’ll notice gradual reduction in swelling and discomfort, with most acute symptoms resolving within the first 10 days.
Osseointegration — the process by which bone grows around and bonds with the titanium implant surface — represents the critical phase determining long-term success. This biological process occurs gradually and invisibly, with new bone formation beginning within days but requiring months to achieve full maturity. Upper jaw implants typically need 4-6 months for complete integration, while lower jaw implants may be ready in 3-4 months due to denser bone structure.
After successful osseointegration, the final restoration phase begins with uncovering the implant and placing an abutment — the connector piece between implant and crown. This minor procedure requires only local anesthesia and brief healing time. Crown fabrication and placement typically add another 2-3 weeks to the timeline, bringing the total treatment duration to 4-7 months from initial surgery to final restoration completion.
What Factors Influence Dental Implant Success?
Beyond surgical technique and patient health, several factors significantly impact both immediate healing and long-term implant survival. Bone quality and quantity at the implant site provide the foundation for success, with adequate width, height, and density ensuring proper support. When natural bone is insufficient, bone grafting procedures can create the necessary foundation, though this extends the treatment timeline and requires additional healing phases.
Systemic health conditions profoundly influence healing capacity and implant integration. Diabetes, when well-controlled with hemoglobin A1c levels below 7%, generally doesn’t impair success, but uncontrolled diabetes dramatically increases failure risk. Autoimmune conditions requiring immunosuppressive medications may slow healing and increase infection risk, requiring modified protocols and closer monitoring throughout treatment.
Post-surgical care and long-term maintenance habits largely determine implant longevity beyond the initial healing period. Meticulous oral hygiene, regular professional cleanings, and routine monitoring help prevent peri-implantitis — the leading cause of late implant failure. Smoking cessation remains one of the most impactful steps patients can take, as continued tobacco use doubles the risk of complications and implant loss.
The evolution of implant surface technologies and digital planning tools continues improving success rates and reducing treatment times. Modern implant surfaces promote faster osseointegration, while 3D treatment planning ensures optimal positioning and reduces surgical complications. For patients considering this investment in their oral health, understanding these success factors helps optimize outcomes and provides realistic expectations for what promises to be a decades-long solution to tooth loss.