The American Dental Association’s 2024 clinical guidelines indicate that 178 million Americans are missing at least one tooth, while 40 million have lost all their teeth — numbers that continue climbing as the baby boomer generation reaches their 70s and 80s. What’s changed dramatically isn’t just the scale of tooth loss, but the sophistication of replacement options available today. Modern dental technology has transformed both implant procedures and denture materials, creating more durable, comfortable alternatives than ever existed before.
For adults facing tooth loss — whether from decay, gum disease, or injury — the decision between implants, dentures, and other alternatives carries long-term consequences for oral health, daily comfort, and bone preservation. The stakes extend beyond aesthetics: untreated tooth loss accelerates jawbone deterioration and can compromise remaining teeth within months. Understanding how these replacement options work differently, which patients benefit most from each approach, and what newer alternatives offer can guide you toward a decision that supports your oral health for decades ahead.
What Happens to Your Oral Health When Teeth Are Missing
Missing teeth trigger a cascade of changes that most people don’t anticipate until they’re already underway. The most critical involves bone loss — when tooth roots no longer stimulate the jawbone through chewing pressure, the bone begins resorbing within just three to four months. This creates a domino effect: as bone shrinks, neighboring teeth shift toward the gap, potentially creating bite problems and making those remaining teeth harder to clean effectively.
Consider someone who loses a molar and decides to “wait and see” rather than pursue immediate replacement. Within six months, the opposing tooth in the other jaw may begin over-erupting into the space, while adjacent teeth tilt inward. The altered bite pattern places unusual stress on other teeth, increasing their risk of fracture or additional loss. Meanwhile, the shrinking jawbone in that area becomes increasingly difficult to restore later — what might have required a straightforward implant initially could eventually need bone grafting or more complex reconstruction.
The functional impacts compound over time. Speech patterns adapt around missing teeth, sometimes creating permanent changes even after replacement. Chewing efficiency drops significantly with each lost tooth, particularly molars, forcing people to avoid certain foods or inadequately chew others before swallowing. Research from the Journal of Prosthetic Dentistry shows that individuals missing multiple posterior teeth often develop nutritional deficiencies from avoiding harder-to-chew proteins and fibrous vegetables.
Beyond the mechanical problems, missing teeth affect facial support structure. The lips and cheeks lose underlying support, creating a sunken appearance that can age someone’s face considerably. This happens gradually but becomes irreversible once significant bone loss occurs, making the timing of replacement decisions more crucial than many people realize.
How Do Dental Implants and Dentures Work Differently
Dental implants function by replacing the tooth root itself — a titanium post surgically placed into the jawbone that fuses with bone tissue over three to six months through a process called osseointegration. Once healed, the implant provides a foundation for a crown that looks and functions like a natural tooth. The surgical procedure typically involves local anesthesia, precise drilling to create space for the implant, and careful placement at specific depths and angles. Most patients experience moderate discomfort for a few days, then normal function returns as healing progresses.
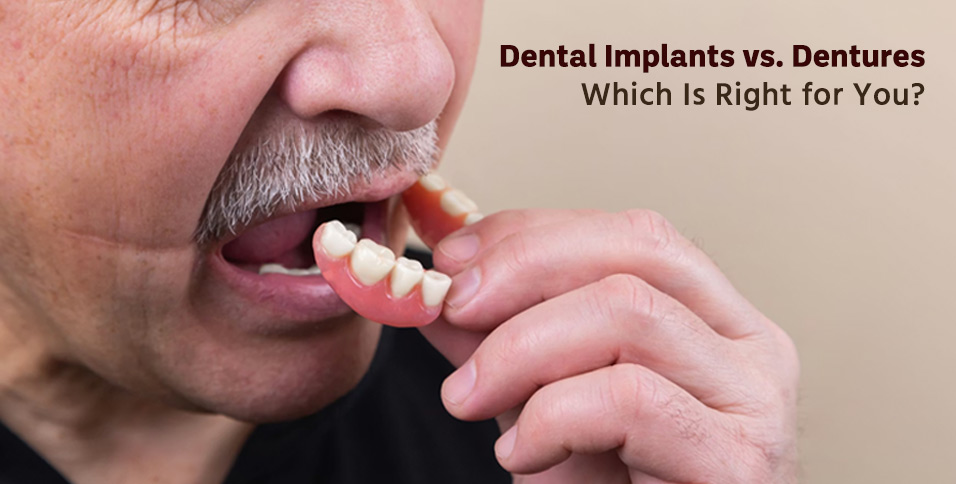
Dentures take an entirely different approach, resting on the gum surfaces and relying on suction, muscle control, and sometimes adhesive for retention. Complete dentures replace all teeth in an arch, while partial dentures fill gaps between remaining natural teeth using clasps or precision attachments for stability. The fitting process involves taking detailed impressions, creating custom bases that distribute chewing forces across the gums, and multiple adjustment appointments to achieve proper fit and function.
The patient experience differs substantially between these approaches. Implant treatment typically requires two to four appointments over several months — initial consultation, surgical placement, healing period, then crown attachment. During the healing phase, patients usually wear temporary restorations and follow specific care protocols to ensure proper integration. The process demands patience but results in teeth that feel completely natural once completed.
Denture patients face a more immediate but ongoing adjustment process. New dentures often feel bulky initially and may cause sore spots as the mouth adapts. Eating requires relearning techniques — cutting food smaller, chewing more slowly, avoiding sticky or very hard foods that might dislodge the appliance. Speech may sound different for several weeks as the tongue adapts to the new oral environment. Even well-fitted dentures need periodic adjustments as the underlying bone and gum tissue continues changing over time.
The daily maintenance routines also diverge significantly. Implants integrate into regular brushing and flossing habits with minimal additional care, while dentures require removal for cleaning, special soaking solutions, and careful handling to prevent damage from drops.
How Do Success Rates and Patient Candidacy Vary Between Options
Modern dental implants demonstrate remarkable longevity when properly placed and maintained, with success rates exceeding 95% over 10 years according to the International Congress of Oral Implantologists. However, success depends heavily on patient factors that don’t affect denture candidacy. Adequate bone density and volume are essential — patients who’ve been missing teeth for extended periods often need bone grafting procedures before implant placement becomes viable.
Certain medical conditions significantly impact implant success while having minimal effect on denture treatment. Uncontrolled diabetes can impair healing and osseointegration, while medications like bisphosphonates (used for osteoporosis) increase risk of jawbone complications. Heavy smoking reduces implant success rates to around 85% due to impaired blood circulation and healing response. These same factors rarely prevent someone from wearing dentures successfully.
Age considerations work differently for each option. While there’s no upper age limit for implants in healthy patients, the healing process may extend longer in older adults. Conversely, very young patients whose jawbones are still developing aren’t candidates for implants until growth completes, typically around age 18-21. Dentures can accommodate patients at any age once adult teeth are lost.
For individuals seeking affordable implant solutions, candidacy often comes down to balancing bone quality, healing capacity, and long-term oral health goals. Patients with good bone density and general health typically achieve better outcomes with implants, while those with significant medical complexities or extensive bone loss might benefit more from denture treatment.
Financial considerations also influence candidacy in practical terms. Implant treatment typically costs more upfront but may prove more economical over decades due to durability and minimal maintenance needs. Dentures cost less initially but require periodic replacement — conventional dentures typically last 5-7 years before needing replacement due to wear and continued bone changes.
The lifestyle factors matter as well. Patients who prioritize eating a varied diet, maintaining active social lives, or work in professions requiring clear speech often find implants worth the additional investment and treatment time. Those seeking the quickest return to function or who have concerns about surgical procedures might prefer denture treatment despite the ongoing adjustments required.
What Are the Pros and Cons of Dental Bridges and Other Alternatives
Types of Dental Bridges and When They Are Used
Fixed bridges offer a middle ground between implants and dentures by anchoring replacement teeth to adjacent natural teeth. Traditional bridges require crowning the neighboring teeth to serve as anchors, making this option most appropriate when those teeth already need restoration due to decay or large fillings. The process typically takes two to three weeks — first appointment for preparation and impressions, second for placement of the custom bridge.
Resin-bonded bridges, sometimes called Maryland bridges, attach to the backs of adjacent teeth with minimal tooth preparation required. These work best for replacing front teeth where chewing forces are lighter, particularly in younger patients with strong adjacent teeth. The conservative approach preserves healthy tooth structure but limits long-term durability compared to traditional bridges.
Implant-supported bridges combine the advantages of implant stability with the efficiency of replacing multiple adjacent teeth. Instead of placing individual implants for each missing tooth, two or three strategically positioned implants can support a bridge replacing four to six teeth. This approach reduces surgical time and cost while providing excellent stability and bone preservation benefits.
Bridge treatment works especially well for patients who want fixed, non-removable teeth but aren’t ideal implant candidates due to bone loss or medical factors. The success depends heavily on the health and stability of the anchor teeth — if these supporting teeth develop problems later, the entire bridge may need replacement.
Non-surgical Alternatives Beyond Dentures and Bridges
Removable partial dentures offer the most conservative approach for replacing multiple teeth, using clasps or precision attachments to secure to remaining natural teeth. Modern materials have improved significantly — flexible partial dentures made from thermoplastic materials provide better comfort and aesthetics than traditional metal-clasp designs. These work particularly well for patients missing several teeth in different areas of the mouth.
Orthodontic space closure represents an overlooked alternative for certain cases, particularly single missing teeth in younger patients. By moving adjacent teeth together to eliminate the gap, orthodontic treatment can restore function and appearance without requiring any prosthetic replacement. This approach takes 12-18 months but preserves all natural tooth structure while improving overall alignment.
Mini implants provide a less invasive implant option for patients with limited bone or who want to avoid major surgery. These smaller-diameter implants can often be placed without bone grafting and may support small crowns or help stabilize loose dentures. While not as durable as conventional implants for heavy chewing forces, mini implants serve well for front teeth or denture support applications.
Snap-on dentures, also called overdentures, combine removable convenience with implant stability. Two to four implants placed in the jaw provide anchor points for special attachments that secure the denture firmly during eating and speaking, while still allowing removal for cleaning. This hybrid approach reduces the slipping and discomfort common with conventional dentures while costing less than full implant reconstruction.
How Can You Maintain Oral Health After Tooth Replacement
Successful long-term outcomes depend more on daily maintenance habits than on the initial treatment choice. Implant patients must commit to meticulous cleaning around the implant site — bacterial buildup can cause peri-implantitis, an inflammatory condition that destroys the bone supporting the implant. This requires special interdental brushes, water flossers, or other tools designed to clean beneath the crown margin where regular toothbrushes can’t reach effectively.
Denture wearers face different but equally important maintenance requirements. Removing dentures each night allows gum tissues to recover from daytime pressure and enables thorough cleaning of both the appliance and remaining oral tissues. Soaking in antimicrobial solutions helps prevent bacterial and fungal growth, while proper handling during cleaning prevents damage from drops or aggressive scrubbing.
Bridge maintenance falls somewhere between natural teeth and implants in complexity. The connection points where crowns meet gums require extra attention, and cleaning beneath the replacement tooth (pontic) demands floss threaders or specialized cleaning devices. Regular dental cleanings become more critical since bacterial buildup around bridge margins can compromise the supporting teeth.
Regardless of the replacement method chosen, protecting remaining natural teeth becomes paramount. The altered chewing patterns that develop around any prosthetic device can place unusual stress on other teeth, making them more susceptible to fracture or excessive wear. Using night guards, avoiding extremely hard foods, and maintaining consistent professional dental care help preserve the overall oral health that supports any replacement option.
The most successful patients develop cleaning routines immediately after treatment completion and stick with them consistently. Whether that involves daily implant-specific cleaning tools, nightly denture care, or modified bridge hygiene techniques, the time invested in proper maintenance typically determines whether tooth replacement lasts five years or several decades.